Viral Infections
COVID-19 demonstrated that respiratory viruses can damage olfactory neurons. Other common viruses do the same, often with better recovery than COVID-related cases when addressed early.

Food tastes like nothing. Coffee has no aroma. You have been told it will come back on its own, yet months or even years have passed with no improvement. Meals feel hollow. Social gatherings around food leave you feeling isolated. Dr. Ashley Prince developed a protocol that targets the neurological pathways other treatments miss entirely.
Anosmia rarely arises from a single event. These are the most common drivers we identify during evaluation across our conditions practice in The Woodlands.
COVID-19 demonstrated that respiratory viruses can damage olfactory neurons. Other common viruses do the same, often with better recovery than COVID-related cases when addressed early.
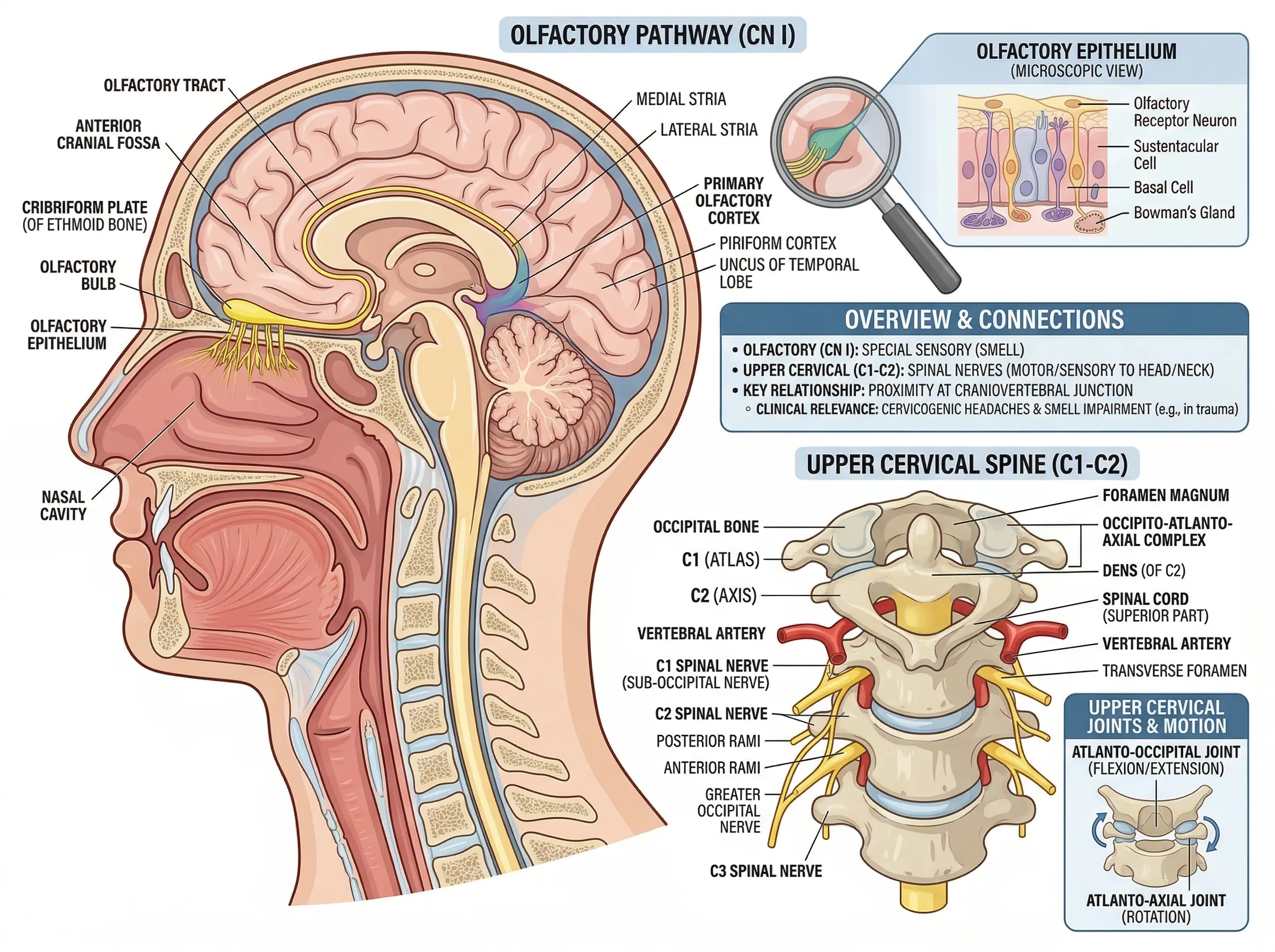
Concussion or traumatic brain injury can shear the delicate olfactory nerves where they pass through the cribriform plate. Loss may appear immediately or weeks after the original event.
Polyps, chronic sinusitis, and septal deviation block air from reaching the olfactory cleft. Treating the structural blockage often restores function once airflow is reestablished.
Industrial solvents, pesticides, and household chemicals damage olfactory receptors. Cumulative low-dose exposure matters as much as a single high-dose event for long-term function.
Antibiotics, antihistamines, antidepressants, and chemotherapy regimens alter taste and smell as a documented side effect. A medication review is part of every workup.
Parkinson's, Alzheimer's, and multiple sclerosis can present with olfactory loss years before classic symptoms. Smell testing is now used as an early indicator of underlying neurological disease.
Loss of smell affects far more than the ability to detect odors. The neurological disruption behind anosmia produces sensory, emotional, and safety-related symptoms that change daily life.
"The world becomes flat. You eat for fuel. You walk past a bakery and feel nothing. Conversations about food sound like a foreign language. Anosmia is not a quirk to wait out. It is the steady erasure of a sense that connects you to memory, safety, and the people you love."
Most ENTs will tell you to wait. They may suggest olfactory training or a steroid course, then send you home with no clear timeline. Dr. Ashley Prince developed a protocol featured on every major US news network that targets the neurological pathways other treatments miss. Patients travel from across the country for this care.
Dr. Prince's upper cervical technique has been featured on every major US news network. Hundreds of patients have traveled from across the country for this treatment, making Prince Health a national destination for sensory recovery.
The protocol targets the upper cervical spine and cranial nerve pathways that influence olfactory function, addressing the structural nerve interference that disrupts sensory signal transmission at its source.
Progress is documented through standardized sensory testing at each visit. You will see measurable improvement in olfactory and gustatory function rather than relying on subjective guesswork or vague reassurance.
Anosmia is the complete loss of the sense of smell, often accompanied by reduced taste, since both senses share neurological pathways. Treated at Prince Health with Dr. Ashley Prince's nationally recognized Taste and Smell Recovery Protocol to restore sensory function through targeted upper cervical correction.
The medical terminology distinguishes four related conditions. Anosmia is the complete loss of smell. Hyposmia is a reduced or partial loss. On the taste side, ageusia is the complete loss of taste, while hypogeusia is a partial loss. Most patients fall into combinations rather than a clean total loss of either sense, and identifying which category you actually fall into shapes the right evaluation and recovery plan.
The olfactory nerve carries signals from receptors in the nasal cavity to the olfactory bulb in the brain. Inflammation, swelling, or nerve damage anywhere along this pathway can diminish or eliminate the ability to smell. Taste follows closely. The two senses are neurologically intertwined, which is why patients who lose their sense of smell almost always report that food tastes flat, metallic, or absent.
COVID-19 brought global attention to anosmia, yet viral infections, chronic sinus disease, head trauma, toxic chemical exposure, and neurological conditions have caused this condition for decades. The difference today is that more people are living with prolonged sensory loss and fewer solutions exist in conventional medicine. Steroids may reduce inflammation temporarily. Olfactory training can help some individuals. Neither addresses the structural nerve interference that often sustains the problem.
Parosmia and phantosmia share the same underlying nerve dysfunction. Parosmia distorts familiar smells into unpleasant or unfamiliar odors. Phantosmia creates the perception of smells that do not exist in the environment. Both suggest active nerve misfiring rather than complete nerve silence. Both respond to the same upper cervical approach we use for anosmia, and our evaluation flags whether either pattern is present alongside related conditions like long COVID.
Our treatment for anosmia centers on Dr. Ashley Prince's nationally recognized protocol, tailored to your specific cause, symptom duration, and sensory baseline.
Four steps from first visit to documented sensory recovery. The same protocol every patient receives, regardless of how long their loss has lasted.

Detailed history of your olfactory and gustatory loss including onset, duration, suspected cause, and prior treatments. Upper cervical assessment and cranial nerve screening.

Validated smell and taste testing establishes your current level of function and creates a measurable baseline so progress can be documented in objective numbers, not feelings.
A protocol built around Dr. Prince's upper cervical technique, with frequency and duration calibrated to the severity, cause, and duration of your sensory loss.

Standardized retesting at each milestone documents objective improvement in olfactory and gustatory function. The plan adapts to your data, not assumptions about typical recovery.
Schedule your evaluation with Dr. Ashley Prince at Prince Health in The Woodlands, TX. Our nationally recognized protocol has helped hundreds of patients recover sensory function.
Loss of taste and smell most commonly results from COVID-19 inflammation of the olfactory nerve, but can also stem from sinus conditions, head trauma, or neurological causes. The olfactory nerve pathway runs through the upper cervical region, which is why spinal alignment plays a role in recovery.
The protocol targets upper cervical spinal alignment and cranial nerve pathways that influence olfactory function. By restoring proper nerve signaling through specific chiropractic techniques, the body can begin recovering sensory function. Dr. Prince has been featured on major national news networks for this work.
Recovery timelines vary widely. Some patients regain function within weeks, while others experience months of reduced sensation. Our protocol has helped patients recover function even after prolonged loss. Earlier intervention typically produces faster results.
Yes. Olfactory training, where you deliberately practice smelling specific scents daily, can complement our chiropractic approach. We may incorporate this into your treatment plan alongside spinal correction for a more complete recovery strategy.
The protocol uses gentle, non-invasive chiropractic techniques that can be adapted for most patients. We evaluate each person individually to confirm they are a good candidate. The approach involves no medication, no surgery, and no known adverse effects.
Treatment costs depend on the number of sessions needed and the complexity of your case. We provide pricing details during your initial consultation. Patients travel from across the country for this protocol because the results are not available through conventional approaches.
Not necessarily. Many cases involve inflammation or misalignment that disrupts nerve signaling rather than permanent nerve damage. The distinction matters because functional disruption can often be corrected, while structural damage requires a different approach. Our evaluation determines which category your condition falls into.
Anosmia is often the first signal of a deeper post-viral or inflammatory process. These are the related conditions we frequently uncover alongside taste and smell loss.

Multi-modal approach to persistent post-COVID symptoms through hyperbaric oxygen therapy, IV therapies, functional medicine evaluation, and nervous system restoration.

Comprehensive evaluation and multi-modal treatment for acute and chronic Lyme disease through functional medicine, IV therapies, and immune system support.

Comprehensive evaluation and treatment for mold-related illness through functional medicine testing, detoxification protocols, and IV therapies.

Comprehensive management of chronic EBV reactivation through functional medicine evaluation, immune support, and targeted therapies including IV ozone and SOT.
Our office is located at 10847 Kuykendahl Rd #350 in The Woodlands, TX 77382, easily accessible from Woodlands Parkway, Kuykendahl Road, and the I-45 corridor.
We serve patients from Alden Bridge, Cochran's Crossing, Creekside Park, Sterling Ridge, Panther Creek, Grogan's Mill, and surrounding communities.
10847 Kuykendahl Rd #350
The Woodlands, TX 77382
Schedule your appointment at Prince Health in The Woodlands, TX. We listen first, evaluate thoroughly, and build a plan that fits your goals.